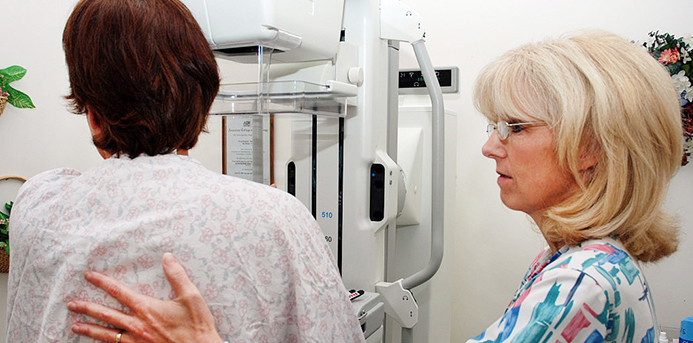
Breast cancer is the cancer with the highest incidence among women, regardless of race or ethnicity, according to the Centers for Disease Control (CDC).
Many people are aware of the disease, but not what they can do to reduce their risk. “We strongly encourage women to take steps to reduce their risk of breast cancer,” says Maryann Rasmussen, senior market manager of the Lakeshore Division of the American Cancer Society (ACS). “Prevention is much easier than having to treat or cure cancer.”
Breast cancer experts shared a few of the many risk factors for breast cancer and ways women can manage them to keep their risk as low as possible.
Vitamin D Deficiency
Many people associate exposure to the sun with an increased risk of skin cancer, but by staying inside and covered up, many people are missing out on the vitamin D that comes from spending time outside, and that can elevate the risk of other cancers, including breast cancer.

Dr. Eugene Ahn, medical oncologist at Cancer Treatment Centers of America at Midwestern Regional Medical Center, calls the prevalence of vitamin D deficiency a “silent epidemic.”
“Fifty percent of women in the United States are vitamin D deficient, with 75 percent of women in the Midwest having a deficiency,” he explains, noting that greater time spent indoors and out of the sun is perhaps partly fueled by fear of elevated cancer risk, but staying inside may not be the answer.
“A recent study showed that the top third of people with the most sun exposure even accounting for skin cancers had the least cancer risk, and those in the bottom third had equivalent cancer risk to active smokers,” he explains.
Ahn suggests women get a simple blood test to check their vitamin D25 level and speak with their physician regarding the appropriate level of vitamin D for them. A supplement can often correct a deficiency without increasing exposure to UV rays.
Alcohol Intake
You may want to think twice before raising a second glass given that doing so often could increase your breast cancer risk.
“Numerous studies have demonstrated that the intake of moderate amounts of alcohol, one to two drinks per day, is associated with an increased risk of breast cancer,” says Dr. Dean Tsarwhas, medical director of oncology services at Northwestern Medicine Lake Forest Hospital and Northwestern Medicine Grayslake Outpatient Center.
Dr. Catherine Pesce, a breast surgeon at NorthShore University HealthSystem, says, “Data on alcohol shows that it is okay in moderation, meaning no more than two to three drinks per week.” One drink equals one ounce of liquor, six ounces of wine or eight ounces of beer.
Dense Breasts
Women with dense breasts are more likely to get breast cancer, and it can also be harder to detect tumors in dense breasts via mammogram, according to the CDC. Dense breasts are common and not abnormal, says Tsarwhas.
There are four levels of breast density, with one being the least dense and four being the densest, with the least amount of fatty tissue. “In groups three and four, it is known that mammograms are not as good and can miss things,” says Pesce.
Women cannot control their breast density, which declines with age. Being aware of it, however, enables women to make informed screening decisions with their doctors. Laws in some states require that women be told if their breasts are dense.
At NorthShore University HealthSystem, women in groups three and four can have automated whole breast ultrasound. “Our experience with it has been incredible,” says Pesce. “We have found breast cancers in women that mammograms have missed when they were very small, easily treatable and curable.”
Ahn also notes that women with dense breasts should “be aware that MRI is considered a better imaging surveillance strategy than mammograms, but it comes with its own caveats, particularly higher risk of false positives and unnecessary biopsies.”
He adds, “Women with dense breasts can certainly take to heart the advice on reducing their risk, especially staying physically active, eating a diet less exposed to animal fat and limiting alcohol intake. Since the relative impact of each of those interventions is considered uniform for all people, the absolute impact for a woman with dense breasts would be expected to be even higher.”
Hormone Therapy
“Current or prior estrogen and progesterone hormone therapy is linked to a higher risk of breast cancer,” says Tsarwhas. “Estrogen therapy alone without progesterone, used in women who have had a prior hysterectomy, is not associated with an increased risk of breast cancer.”
He advises women to weigh the possible risks and benefits with their doctors and says factors to consider include a woman’s baseline risk of breast and other cancers, risk of other medical conditions and bone health.
Diet and Exercise
You are what you eat, and body weight and diet can both impact an individual’s risk for any cancer and specifically breast cancer, particularly when it comes to weight gain after menopause, according to breastcancer.org.
“There is no magic diet that can prevent cancer, but there are general recommendations that are very logical, such as eating lots of fruits and vegetables and whole grains and having only lean protein and not much red meat,” says Pesce.
Obesity and inactivity are also known risk factors for breast cancer, according to Ahn. Physicians also stress that maintaining a healthy lifestyle and staying physically fit have tremendous benefits, both in terms of reducing cancer risk as well as promoting good cardiac health and overall well being.
Menstruation Starting Before Age 12
Women who started their periods prior to age 12 have a higher risk of breast cancer later in life, according to breastcancer.org, but the experts found the increased risk to be minimal and not a cause for much concern.
“The general concept is that unopposed estrogen with less progesterone increases risk of breast cancer. Theoretically, this trend you describe would increase risk of breast cancer, but the degree of increased risk is relatively small and probably far dwarfed by the positive impact of healthy lifestyle choices,” explains Ahn.
One Thing You Don’t Have to Worry About: Deodorant
The physicians all say patients have asked about how the use of deodorant affects risk of breast cancer, and they all agree that it is strictly a myth that deodorant use causes breast cancer.
Why It’s Important to Try to Control Your Risk
Unfortunately, not all risk can be controlled. Pesce notes that she has seen breast cancer patients of all shapes and sizes. “Breast cancer does not discriminate,” she says, but adds that it is not a reason for women to give up on controlling their risk. “I will always be a promoter of a healthy lifestyle. It’s always good to be doing something rather than nothing.”
Tsarwhas agrees. “When it comes to our health, sometimes events happen despite our best efforts, and we don’t always have control,” he says. “This shouldn’t dissuade us from trying to live as healthy a lifestyle as possible and to remain up-to-date with recommendations for screening and surveillance.”
Donate to the American Cancer Society:
[takeaction targettype=”org” targetid=”american-cancer-society”]