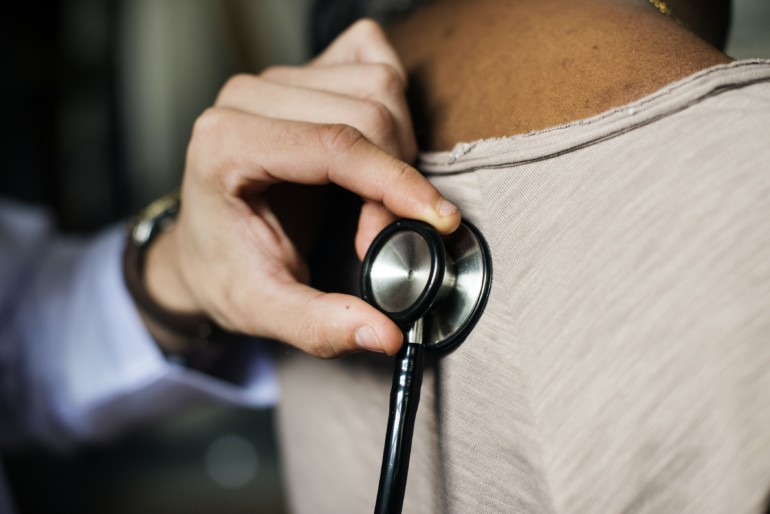
As part of our “You Said It” Op-Ed series, we invite contributors to submit their opinion pieces. Have a submission? Contact us here.
With the new year launched and health care resolutions in place, many are scheduling remote and in-person visits with their doctors. Some are perhaps switching insurance companies and need to find new primary care physicians within network to avoid high costs.
Choosing the right physician is the important first step in improving health. Beyond asking friends and family for recommendations, first impressions at the appointment are crucial.
As a physician, I try to make the most of each visit with a patient for their best health outcomes.
Recently one of my patients has refused to take blood pressure medications for his hypertension over the past three years. I have taken a variety of approaches from fear about the consequences such as heart attack and stroke or imploring him to think of his family, among others. Over time, I built trust and rapport with him.
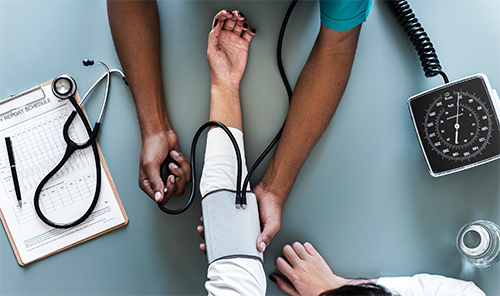
So at his most recent visit, knowing he loved U.S. history, I tried a new approach. I had recently read about the final years of President Franklin Delano Roosevelt, so I showed him the graphic of FDR’s blood pressure during this final years of life.
It tracked perfectly with my patient’s own blood pressure. It also showed how it ended with FDR dying of a hemorrhagic stroke, a common complication of high blood pressure. In a move that surprised me, he asked about potential medications for the first time. This was a huge step forward which would have not happened without years of trust we had formed. It was incredibly rewarding for myself as a physician, but more importantly treatment means he could have more time with his grandchildren.
Here are six keys to making sure your choice of doctor and your regular visits go as well as they can.
1. Schedule early in the day.

Evidence suggests physicians are more proactive with health screenings in the morning, compared to the afternoon. Schedule your appointment as early in the day as possible. The amount of time spent with patients has remained unchanged over the last over the past 20 years; on average physicians spend 10-20 minutes face to face with patients. The electronic healthcare record has not reduced time with patients, but instead just increased time for indirect patient care. This is a major contributing factor to burnout in physicians. Higher burnout leads to fatigue in physicians especially as the day goes on.
2. Avoid physicians who are quick to order tests.

If a physician recommends a test, ask them what medical conditions are they looking for. How will the test result determine or change treatment options? If there is no good answer to these questions, refuse the test. It will only lead to unnecessary cost and potential harm to you. It is estimated that the US spends $75 -100 billion annually on overtreatment and low-value care.
3. Be wary of “routine” labs.
No medical organization recommends them. Unnecessary tests just lead to more unnecessary tests. This “cascade of tests” will only hurt patients in the long run. There is wide variation of testing in primary care practices. Find a physician who is thoughtful about their testing decisions.
4. Ask questions.

When discussing treatments with a physician, the approach should go beyond simply side effects. It is important to ask how the treatment will improve quality and length of life. Ask how long does the medication needs to be taken to get that benefit. In my own practice, online visual aids are helpful to explain benefits and harms for potential treatments. The physician should be able to explain it in clear terms, otherwise, refuse the treatment.
5. Learn more about cancer screenings.
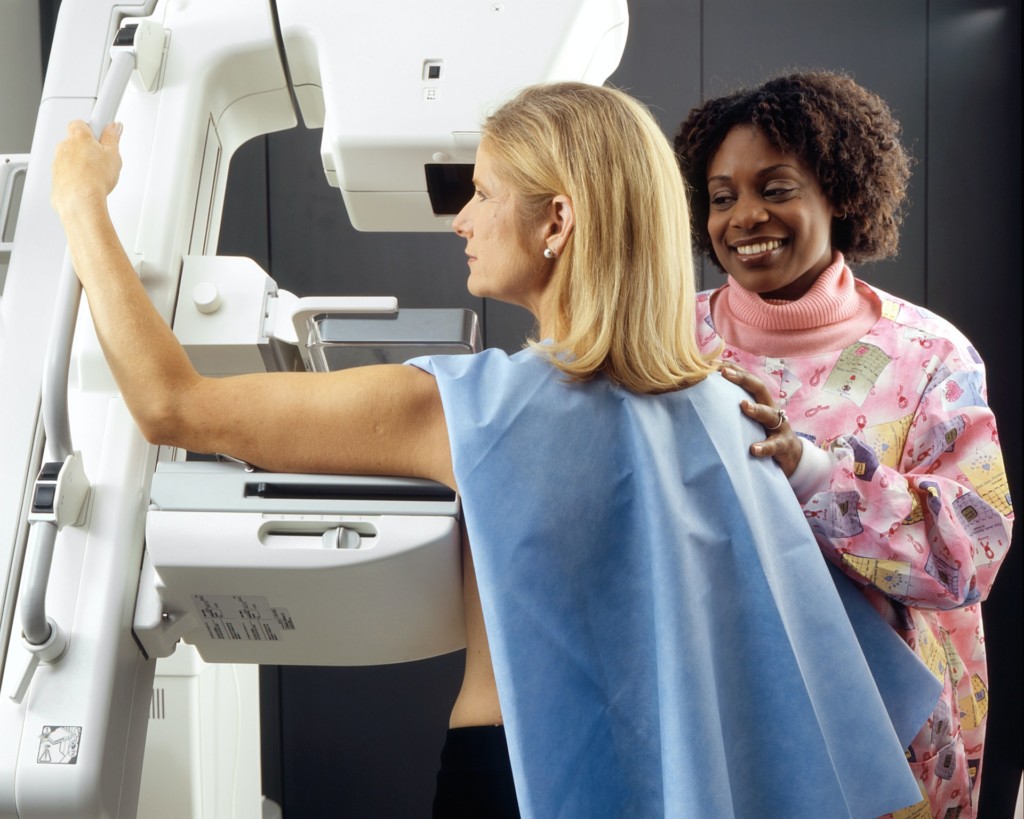
Cancer screenings are a contentious issue and different organizations have different recommendations. For example, The American Cancer Society recommends breast cancer screening starting at age 40 while the United States Preventive Task Force recommends age 50. In 2018, ACS recommended starting colon cancer screening at age 45 from the previous age 50. While it is tempting to think these expansions means an improvement in health, the truth is more complicated. Kidney, thyroid, and skin cancers diagnosis have only increased while mortality has stayed steady the past 40 years. Breast cancer mortality has decreased perhaps reflecting better treatment while incidence has increased reflecting likely overdiagnosis. Colon cancer screening has led to mortality reduction, but lung cancer mortality reduction is likely related to anti-smoking campaigns. Ask the physician if the cancer screening they recommend will extend life in a meaningful way. If they are not sure, hold off until there is a clear understanding of benefit.
6. Visit more than once a year.

The yearly “physical exam” is not helpful. Do not think of a physician visit as a check up, but instead a check in. Develop a relationship with the physician. The trust formed with a committed primary care physician is an invaluable tool for any potential health issues down the road.
Understand that the physician’s goal is to help all of a patient’s problems, but many times it is not possible. Still, a good physician will always try. Think of the physician as a long-term partner in health. The physician likely cannot fix it all in one appointment, but over a lifetime of care they can change it for the better.
More from Better:
- How to Restore, Revive, and Thrive in 2021
- A Look Inside BIÂN, Chicago’s Newest Luxury Health and Social Club
- Be Kind to Your Mind: 10 Groups and Individuals That Tear Down Mental Health Stigmas

Caspian Kuma Folmsbee M.D. is a graduate of Rush University Internal Medicine residency program. He is currently a practicing general internist at Rush University Internists and also serves as associate program director for the Primary Care County/Rush Internal Medicine Program. When not seeing patients, he is chasing his five year old son Miles. Follow him on Twitter @amuknut